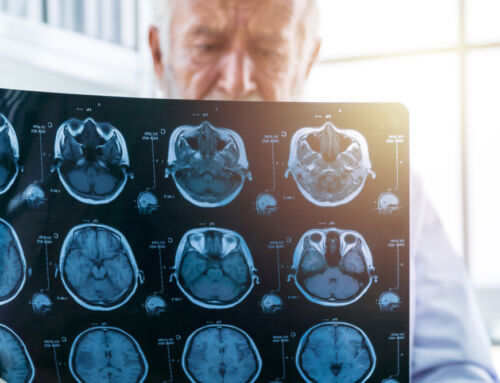
Dementia is not one specific disease. Instead, it’s a general term used to describe a decline in mental capabilities, such as memory issues, that are severe enough to affect activities of daily living (ADLs). Alzheimer’s disease is the most common type of dementia, accounting for around 70 percent of diagnoses, but there are other types too, such as vascular dementia, which occurs after a stroke.
According to the Mayo Clinic, in order to receive a dementia diagnosis, at least two of the following core mental capabilities must be impacted:
- Memory
- Communication and language
- Ability to focus and pay attention
- Reasoning, problem-solving, and judgment
- Visual perception
When words fail us
Many forms of dementia are progressive, getting worse as time goes by. If you have a loved one who has dementia, you may have experienced the communication and language challenges that can accompany the condition and progressively deteriorate over time.
For example, in the early stages of disease, people may have trouble coming up with the right name for a person or word for an object. As they enter the later stages of their condition, they may speak less and less.
>> Related: When Memory Issues Are Cause for Concern
A different approach to communication
This ever-diminishing ability to communicate is one of the reasons that Alzheimer’s and other diseases that cause dementia symptoms have been termed “the long goodbye.” But there are ways to enhance your own communication skills and tactics in order to help better convey comfort and support to a loved one with dementia.
- Be sure to include the person in conversations or discussions that pertain to them, rather than “talking for them.” Always speak to the person with respect.
- Maintain eye contact when talking. If they are sitting, get down to their level.
- Ask your loved one for specific ways that you can help to address their challenges with communication, such as helping them find the right word when they are speaking.
- Refrain from “quizzing” a person with dementia by asking things like, “Do you know where you are?” or “Do you know who I am?” This approach can understandably cause stress and upset for the person, especially if they don’t know the answer. Instead, offer them helpful information, for example saying, “Hi mom, it’s your son, Jim…I’m here to take you to the eye doctor for your check-up.”
- Use simpler, more direct sentences when talking to someone who has dementia, presenting only one concept or instruction at a time. Also, don’t make them feel rushed to respond.
- Especially in the later stages of the disease, use hand gestures and other non-verbal visual cues, like pointing at an object.
Caring for a person with dementia
While the language difficulties that often accompany dementia can make it challenging to communicate, they also underscore the importance of making a plan for the future if you or a loved one receives a dementia diagnosis. Everything from financial and legal issues to safety to long-term daily living concerns must be taken into consideration.
Indeed, there will likely come a time when a person with dementia will no longer be able to live on their own, so one of two scenarios typically will come into play: The person with dementia will either require an around-the-clock in-home caregiver—either a loved one or a paid caregiver—or they will need to be moved to a long-term care facility that includes specialized memory care services.
For some people, providing caregiver services to a loved one is tremendously fulfilling, perhaps allowing them to feel as though they are “repaying” an elder who cared for them when they were a child. But for others, caring for a family member who has dementia can be extremely taxing, leading to physical and emotional exhaustion.
>> Related: Caregiver Assistance- Addressing Caregiver Stress
Specialized memory care
As an alternative to in-home caregiving, memory care communities offer specialized long-term care and housing to seniors with dementia, Alzheimer’s disease, and other conditions that cause cognitive decline. Specially trained caregivers help residents with ADLs and communication issues, and the properties are also well-equipped to manage safety concerns and common symptoms like aggression, confusion, or wandering. Memory care facilities can be free-standing and independently operated, but most are special units contained within a nursing home, assisted living facility, or a continuing care retirement community (CCRC, also called a life plan community).
While not everyone will choose this option to care for a person with dementia, memory care communities can offer a great sense of relief to family members who can feel assured that their loved one is being provided with the safety measures and highly specialized care that is needed by people with dementia.
>> Related: Understanding Memory Loss & Memory Care Communities
The language of love
Coping with the day-to-day realities that go along with having a loved one who has been diagnosed with dementia can be trying, including the decline in language skills, but it is important to remember that much of our communication doesn’t involve actual words at all. A smile, a calm, reassuring tone of voice, holding hands, or a warm hug are all highly effective means of communicating your love for a person with dementia. Simply being present with the person in that moment can be a source of great comfort.
For more information on dementia, including Alzheimer’s disease, the Alzheimer’s Association website has numerous useful resources. To research CCRCs, including communities that offer specialized memory care services, check out our free online community search tool.